By Jana Frances-Fischer, Ph.D.
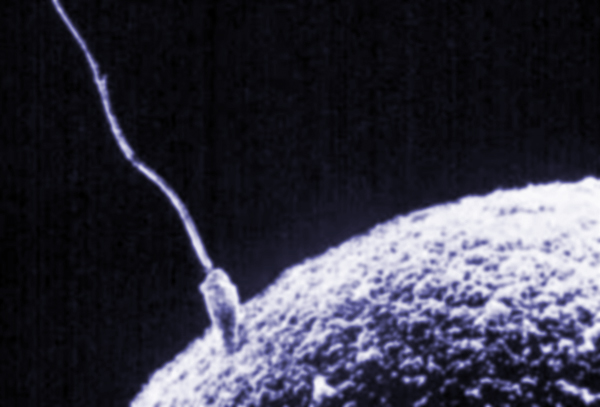
Image source: Wikimedia Commons
When men and their female partners are trying to conceive a child, most probably never expect to encounter fertility challenges. And if reproductive issues become apparent, males often embrace the common myth that infertility exists primarily for women.
When people think about a couple struggling with infertility, commonly, most imagine it ultimately boils down to a “woman’s issue.” Something “wrong” with the female partner is the prevailing view as to the root cause of a couple’s inability to successfully have a child. After all, women are the ones who conceive, experience pregnancy, and eventually give birth.
Research shows us otherwise.
In our current understanding of reproduction, data indicate that “male factors” account for or contribute to about 50% of all medically diagnosed infertility concerns. Therefore, it is particularly important to medically assess men as well as women early on in an infertile couple’s workup.
A number of diagnostic tests are available, but generally male evaluation begins with a semen analysis and possibly a post-coital test and/or other lab work. Further examination and testing by a urologist may also be indicated in certain circumstances. Male infertility can be thought of as the inability to produce adequate healthy sperm leading to successful impregnation of the female partner.
Although a man might be hesitant or even embarrassed to admit to a potential fertility problem, it is equally important that he undergo medical testing as well as his female partner, preferably at the same time, to uncover any male, female, and/or joint infertility factors.
The notion that male factors can contribute to, or are equally responsible for, a couple’s infertility issues may appear very surprising, Yet, besides medical concerns inherent in male factor infertility, it is clear that men also suffer emotionally while in the throes of any stage of infertility: acknowledgement, diagnosis, treatment, and resolution. Because men are typically socialized differently than women, many might “shut down” and not permit themselves to grieve, or openly show the broad range of emotions that woman might feel more comfortable expressing while experiencing infertility. If a man is eventually tested and found to have contributing or even the sole infertility factor, hindering the couple from becoming pregnant, then partner/spouse relationships can become taxed and greatly strained.
Generally, men assume fertility and believe they can easily have their own biological children when and with whom they want them. Often men appear to be in denial and disbelief if and when they are given a medical diagnosis of infertility. Some men might feel like failures, emasculated, or sexually impotent upon learning that their fertility might be a significant factor in preventing a healthy pregnancy. Common emotions experienced by men dealing with their own fertility issues include a sense of loss of control, powerlessness, frustration, inadequacy, and not feeling like a “real man.”
Typically, men are socialized to solve and fix problems with workable solutions. Infertility can frustrate and thwart that logical problem solving process that might work for many other issues in a man’s or couple’s life. Other men might experience a spiritual crisis upon learning of their diagnosis or if medical treatment fails to correct a problem created by male factor infertility. Some might feel angry at God or their higher power, while others might feel guilty or shameful, and may attribute their infertility to punishment over a past transgression.
If treatment is successful, many men might be able to move on, whether their child is biologically related to them or not. If parenthood is eventually achieved, some men might feel closer to their wives and more in touch with their feelings having endured and survived infertility’s many challenges together as a team.
So, although male factor infertility is a “medical” condition, men as well as women can experience a range of strong psychological reactions to it such as anger, denial, guilt, grief, and sadness. The stigmatizing nature of male infertility and its perceived threat to masculinity may compel men to keep their fertility problems a secret, thus removing them from potential support sources that might help lessen their understandable anxiety and strengthen their ability to cope during diagnosis, treatment, and resolution phases.
In some cases, individual or couples therapy or support groups might help men come to trust and empathize with others in the same situation; they can learn to separate issues such as self-worth and virility from the medical condition that is male infertility. Strengthening relationships, reducing a sense of shame and helplessness, and promoting psychological healing and well-being can help many men and couples move beyond their experiences of male infertility.
This article originally appeared in the RESOLVE New England Summer 2008 Newsletter.
